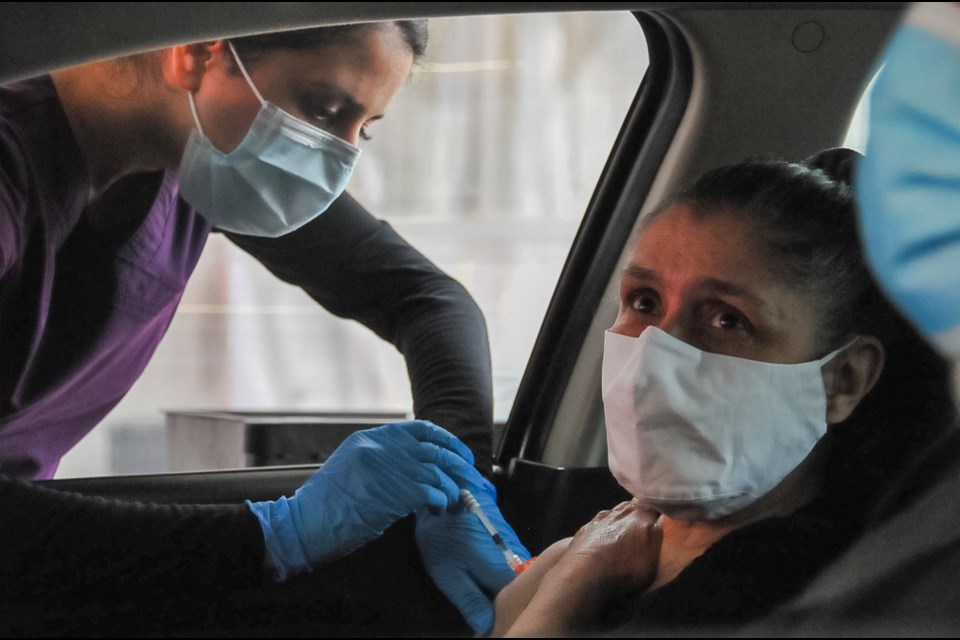
A slow trickle of vehicles snaked through the Coquitlam Centre drive-thru immunization site Wednesday. Rowena Cando, 57, hung out a minivan door smiling through her mask as she rolled up her sleeve; Maria Yule grimaced as the needle slid into her arm before dropping her shoulder in relief.
“I just feel safer. I'm around my kids, my grandkids,” said the Port Coquitlam woman. “It's peace of mind.”
While the delivery of vaccine to such sites has come in spurts — often a product of sporadic deliveries to British Columbia — it’s not clear why so few have been booked for appointments at this drive-thru clinic.
On its busiest days, nurses say they’ve inoculated over 400 people. But while May 5, the day the Tri-City News visited the drive-thru site, was nowhere close to that number, record vaccine shipments are on the way and there are strong signs B.C.’s push toward herd immunity could soon get a major boost.
'KIDS ARE REALLY IMPORTANT'
Earlier on Wednesday, Health Canada announced it had approved the Pfizer-BioNTech vaccine for children 12 and over. Within hours, provincial health officer Dr. Bonnie Henry said she was working on a plan to incorporate B.C. adolescents into the province’s vaccination campaign. B.C. youth aged 12 to 17, she said, could receive a COVID-19 vaccine by the end of the school year, possibly through school clinics.
By the end of Thursday, Dr. Henry said the province will have administered its two millionth dose. But most of those are first doses, meaning roughly 37% of the population has received at least one shot. That's a far cry from the 80 to 90% vaccination rates some experts say is necessary to achieve herd immunity.
Still, the drive to offer vaccine to younger segments of the population has buoyed the hopes of some experts who have expressed skepticism that B.C., and indeed Canada, could reach such high vaccination rates.
“Kids are really important,” said infectious disease expert Caroline Colijn, who leads a multidisciplinary COVID-19 modelling team out of Simon Fraser University.
“There’s enough kids out there that vaccinating 90% of adults, plus 90% of youth makes a big difference.”
Many experts in the United States and Canada have recently gone on the record saying it's unlikely the countries will achieve herd immunity.
Prof. Paul Tupper of Simon Fraser University's mathematics department said herd immunity is unlikely to happen with COVID-19 for a few reasons.
Because the virus is transmitted worldwide, its reintroduction between communities and across borders could hit as immunity through vaccination or infection wears out. To complicate matters, the vaccines don't seem to be completely effective against some of the new variants, he said.
"So, I think what is more likely to happen is that we end up in a situation like we have with seasonal flu," Tupper said.
"We have to live with the flu, and I think something similar is going to happen with COVID."
Sarah Otto, a University of British Columbia professor and expert on the mathematical models of pandemic growth and control, said the disease's reproductive rate is hard to pinpoint, which makes it difficult to establish a herd immunity target.
The reproductive rate is the number of additional people infected by a single person with COVID-19, which has also changed because of the variants, she said.
Canada might also fall short of herd immunity because people can still get infected after vaccination, even if they are less likely to develop symptoms, she said.
"We don't yet know how effective vaccines are at reducing transmission from person to person and that matters a lot," Otto said.
Vaccinated people are getting fewer infections but those who do can still suffer severe symptoms, she said.
"Before the pandemic, we didn't have working vaccines for coronaviruses, so we don't know exactly what the outcomes are going to be,” said Otto. “It's very unusual to have a disease with such wildly differing outcomes, with asymptomatic individuals and severely affected long haulers. How are vaccines going to change that mix? We don't really know why the severe cases are so severe."
A STUTTERED REOPENING
SFU’s Caroline Colijn said reaching the threshold of herd immunity really depends on how you define it.
“Herd immunity is kind of an unclear concept,” she said. “Can we get the risk down that we never see COVID ever? I don’t think most experts or the Canadian public believe that.”
In April, Colijn and Tupper modelled different scenarios probing how British Columbia would emerge from province-wide restrictions as its vaccination campaign moved into the summer and fall.
In a summary of their findings, the two experts warned that by not vaccinating youth and not improving vaccine uptake, “it is likely that 100,000s of British Columbians would become infected or some restrictions would need to be re-introduced and maintained indefinitely.”
Opening up vaccination to youth and eventually children significantly changes that calculation, and could lead to a permanent, if stuttered, lifting of restrictions, said Colijn.
“We’re near that fence,” she said, referring to the possibilities opened up by vaccinating younger cohorts.
For Colijn, getting to herd immunity means an eventual lifting of restrictions, yet public health is still in a constant state of heightened vigilance, stamping out a cluster stemming from a returning traveller or a visiting relative.
But even that limited possibility of success must confront two major sources of uncertainty.
First, writes Colijn and her team in a summary of their latest modelling, we know mRNA vaccines, like Pfizer and Moderna, have shown evidence of being “phenomenally effective in preventing symptomatic disease.” But that was during trials, and it’s not clear how effective these vaccines — as well as others from AstraZeneca and Johnson & Johnson — are at stemming the spread of the virus in the real world.
Second, said Colijn, achieving an imperfect herd immunity is predicated on a virus that doesn’t continue to evolve and find a mechanism to escape the effectiveness of current vaccines.
“It’s not going to be, ‘OK, everything is open, let it rip,’” she said, pointing to flare-ups in past widespread vaccination campaigns. “We should look out for those scary things.”
“But we don’t shut the world down because of measles.”
—With files from the Canadian Press