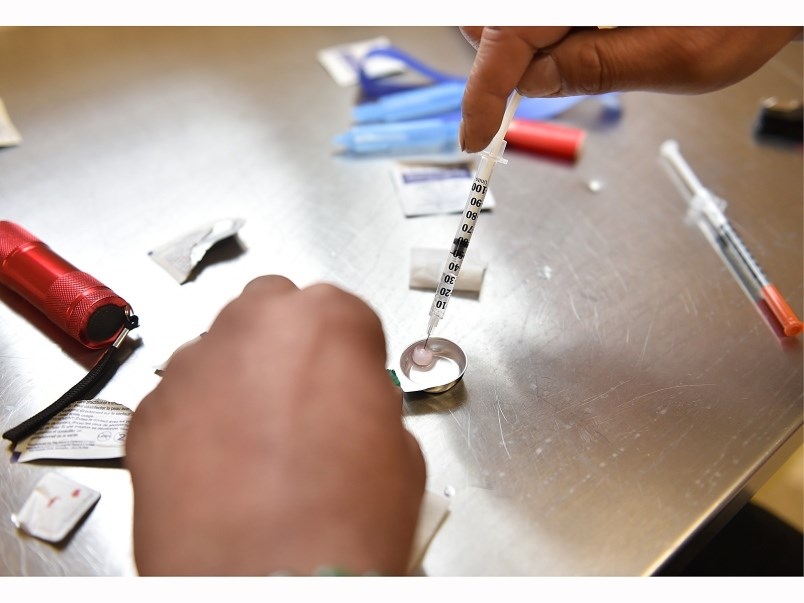
Eagle Ridge Hospital is seeing more patients admitted due to illicit drug overdoses, suggesting the opioid crisis is not over, according to recent figures.
And a local group charged with finding a way to reduce the number of opioid ODs in the Tri-Cities says the community faces unique challenges.
“Things like naloxone are really working,” said Claire MacLean, CEO of Share Family and Community Services, which is leading the group charged with coming up with a local strategy. But the fact that there is still a tainted drug supply and people are at risk is “still a significant issue in our community.”
While the BC Coroner Service is reporting fewer overdose deaths in Coquitlam — nine between Jan. 1 and May 31 compared 20 in 2018 and 30 in 2017 — it appears people are still overdosing but are being revived and taken to hospital.
According to Fraser Health, Eagle Ridge Hospital admitted 169 people with suspected overdoses last year and 91 between January and May 31 this year.
The trend is worrying, MacLean said, but health officials are hoping to see a drop in numbers as the year progresses, as has been seen in other Fraser Health hospitals.
“While there appears to be a slight increase in overdose events in 2019, it is too early to tell whether more overdose visits to the emergency department will continue throughout the rest of the year,” a Fraser Health spokesperson said in an email to the Tri-City News.
Hopes are high that a multi-faceted strategy to address the overdose emergency, with prevention, harm reduction and treatment, will keep people safe even though the drug supply is still tainted with deadly fentanyl.
Numbers so far suggest the strategy may be working, with numbers of suspected overdoses at least stabilizing; there were 2,986 hospital admittances in Fraser Health in 2018 and 1,330 between Jan. 1 and May 31 of this year.
It’s not known how many people are revived from overdoses but not admitted to hospital.
“We know from BC Emergency Health Services, of the overdoses they attend, some people decline transport to the emergency department for follow-up care and monitoring,” Fraser Health spokesperson Aletta Vanderheyden said.
This summer, the local opioid strategy is meeting to plan next steps to deal with the overdose crisis. MacLean said gaps in service have been identified and a coordinator hired to survey agencies and people who use opioids and the next step is to find resources to improve programs and services.
Locally, people who are dying of an overdose tend to be men, and they are dying alone in private residences. Reaching those people is key to reducing the number of overdoses, she said.
In many cases, the men turned to street drugs to deal with pain after their opioid prescriptions ran out; in other instances, someone was experimenting recreationally, perhaps even for the first time, and died because the drug they ingested was tainted with fentanyl or even the stronger carfentanyl.
“It’s about prevention, it’s about de-stigmatization so people can get the help they need, that’s a really strong part of our focus,” MacLean said.