In the early hours of Jan. 15, 2018, Coquitlam resident Neeta Long woke with a bad case of the flu — so bad, her husband, Phil, rushed her to the emergency room at Royal Columbian Hospital.
She had been racked by fever all week when the vomiting started. When she got to the hospital, everything went black.
“The last thing I remember is registering in the ER and walking through the doors,” said Long, who was initially given Gravol and told to go home.
By early afternoon, Long’s condition had rapidly deteriorated. She showed signs of respiratory distress, had difficulty breathing and her kidneys started failing.
Then the test results came back from the lab: Long’s white blood cell count was through the roof and she tested positive for streptococcus A, an invasive bacteria that can lead to serious illness, especially among children and those with compromised immune systems.
But Long was a healthy 39-year-old woman. She worked at Fraser Health in business development, took care of twin 10-year-old boys and volunteered as executive director at their rugby club. What could have triggered such an infection?
Long was rushed to a trauma bay. An intensive care unit (ICU) team inserted a flexible plastic tube down her throat to mechanically ventilate her lungs. All she remembers are flashes of ICU doctors and nurses, their grim faces looking down at her.
Neeta Long was in septic shock and on the cusp of death.
Sepsis, often known colloquially as blood poisoning, is an often misdiagnosed condition because it mimics other illnesses. As the infection spreads through veins and arteries, blood pressure drops, leading to a cascading and catastrophic failure of one organ after another.
Death rates for patients with severe sepsis have been found to be as high as 38% and the condition kills more than 10,000 people every year across the country — representing more than half of all deaths related to infectious diseases — according to Statistics Canada. And because of the difficulty in diagnosing the disease, that number is likely much higher.
After Long's sepsis diagnosis, her organs began to fail. She was put on dialysis and the doctors pumped her full of broad-spectrum antibiotics and a drug called Levophed to boost her blood pressure, which had gotten so low that it triggered three or four minor heart attacks.
Levophed works by drawing blood away from the extremities and towards the body’s organs. Phil Long remembers her feet, hands fingers and toes turning black.
Necrosis, the localized death of living tissue, ascended her legs and arms as they were starved of oxygen. Desperate, Phil Long recorded their two boys’ voices.
“It’s Devon and Cameron,” Long heard her kids say while she lay in an induced coma. “We want you to come home soon.”
“I don’t usually believe in that kind of stuff,” Neeta Long recently told The Tri-City News, but, she added, “That’s when my organs started coming back to life.”
The doctors would soon find the trigger of her compromised immune system, what Long described as a “baseball-sized, pus-filled abscess” in her uterus. Still deep in coma, her flesh dying in her hands and feet, she had a hysterectomy.
The emergency procedures and drugs had saved Long’s life but the hardest days were yet to come.
She spent 10 days in an induced coma, six weeks on dialysis and another nearly eight months in the hospital. Over the first six months, surgeons tried to peel back the dead flesh and save her limbs.
“They waited. My vascular surgeon hoped that my body would heal myself,” she said. “Unfortunately, it was too far gone. My feet were just mummified.”
Six months later, doctors were forced to amputate her left hand and both feet, four and five inches below the knee. Her right hand was so damaged she has taken to calling it a “lobster claw.”
Before sepsis, before the hospital and amputations, Long was set to graduate with a degree in business administration. It would have moved her up the ladder at Fraser Health, she said.
“Then, the next thing you know, you’re just there. It’s changed our life completely,” said Long. “You try to deal with things but it’s a huge shock.”
Still, Long fought on. Her muscles had atrophied after so long stuck in a hospital bed and the sepsis had left her body riddled with large blisters the scars of which still leave her skin hyper-sensitive.
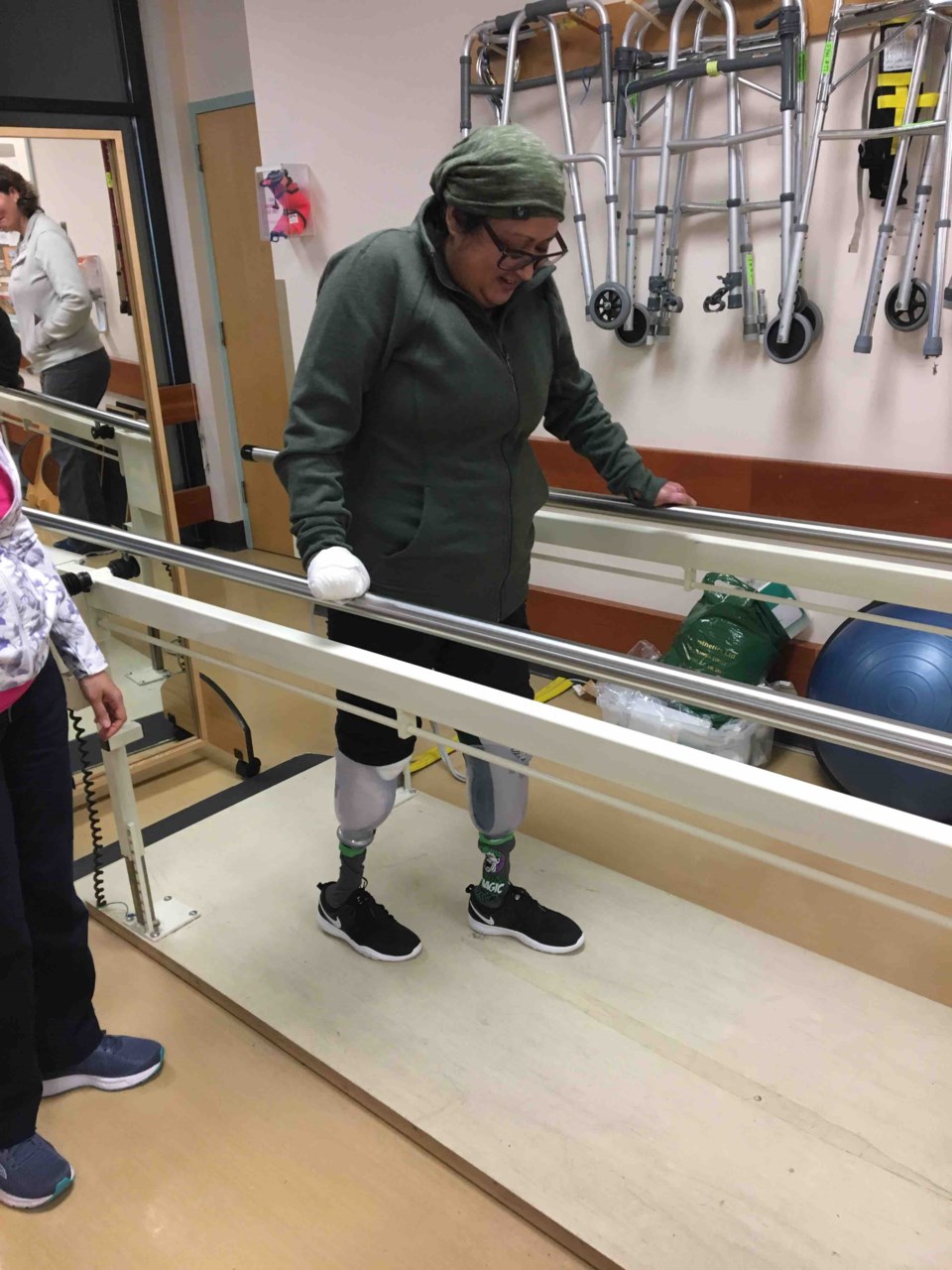
When she received her first pair of prosthetic feet at the end of November 2018 — 10 months after she entered the ER — the process of learning how to walk again, complicated by her painful sores, began.
“It’s amazing how much muscle you lose when you're in bed for 10 months,” she said.
Still, said Long, she was surrounded by her mother, brother, kids and husband, a loving group of people that helped fight back despair.
When her husband, an electrician, took 14 months off work to take care of her, the bills started adding up: $35,000 for a new pair of prosthetics, renovations to make her house accessible, among other mounting costs.
All around the Tri-Cities, people started chipping in. A GoFundMe page started by a friend raised more than $50,000 and a silent auction at Port Coquitlam’s Cat & Fiddle Pub brought in another $14,000. In total, the Longs have received nearly $100,000 in donations from family and friends around the Tri-Cities.
She recently finished a round of physiotherapy for her hand to free what’s left of her fingers from a permanently curled position. The rest, said her physiotherapist, is up to her.
Long’s ambitions, while never fading, have shifted. She still has plans to get back to camping and hiking, although she struggles to walk outside her home. As she builds her strength — and puts aside enough money for the next, articulating pair of prosthetics — Long has started taking online courses at Thompson Rivers University. But instead of business, she’s moved to psychology with the hopes of one day becoming a counsellor and seeing people through their darkest moments.
“It sounds cheesy,” she said, "but I don’t think I survived this to do something that won’t help people.”
“I’m grateful. I could have lost a lot more than I did.”
Correction: An earlier version of this story incorrectly noted 100,000 deaths were attributed to sepsis across Canada every year. Statistics Canada, in fact, attributes over 10,000 deaths to sepsis every year.



